Why Should I Bring my Pet to Willows for Cutaneous Vaculitis?
Willows is one of Europe’s leading small animal referral centres. Our state-of-the-art hospital is led by internationally renowned Certified Specialists who are committed to providing the highest standards of veterinary care. The Dermatology service at Willows is led by Dr Richard Harvey BVSc DVD DipECVD PhD FRSB FRCVS, who works closely with fellow Specialists in the disciplines of Internal Medicine,
Orthopaedics, Soft Tissue Surgery, Neurology, Ophthalmology, Oncology and Anaesthesia. Round the clock veterinary and nursing care is provided to ensure the best possible outcome in each and every case.
What is Cutaneous Vasculitis?
Vasculitis is a term used to describe a variety of skin diseases that are caused when inflammation targets the walls of the blood vessels. In dogs and cats, inflammation tends to affect the small blood vessels of the skin. Vasculitis is not a diagnosis in its own right, as it can be associated with a number of different causes. It is therefore best thought of as a reaction pattern seen within the skin.
What Causes Vasculitis?
The inflammation is thought to be the result of an abnormal immune response. This abnormal response can be triggered by a number of different things. Many drugs have been implicated in the formation of vasculitis, and a thorough drug history is therefore vital in animals where vasculitis is suspected. Vaccines are also responsible for some cases of vasculitis. In particular, a characteristic presentation of vasculitis has been reported following the administration of rabies vaccine. Various infections including bacteria, viruses and protozoa (single celled organisms) have also been implicated in cases of vasculitis and rare cases can be triggered by internal cancer. A subset of cases do not have an identifiable trigger and are termed ‘idiopathic’.
Genetics may well have a part to play in the development of cutaneous vasculitis. In dogs, breeds such as the German Shepherd Dog, Saint Bernard, Jack Russell Terrier, Greyhound and the Chinese Shar-pei appear more prone to vasculitis. Breeds such as the Yorkshire Terrier, Poodle, Silky Terrier and the Maltese Terrier may be more prone to develop vasculitis as a result of vaccination.

What Can I Expect if my Pet has been Diagnosed with Vasculitis?
Vasculitis is a very variable disease; some cases are relatively mild while rare cases can be much more serious. Unless an obvious underlying cause can be identified and corrected, the vast majority of dogs and cats require long term medications for the rest of their lives to control the disease. However, despite this, the prognosis for the majority of cases is usually good.
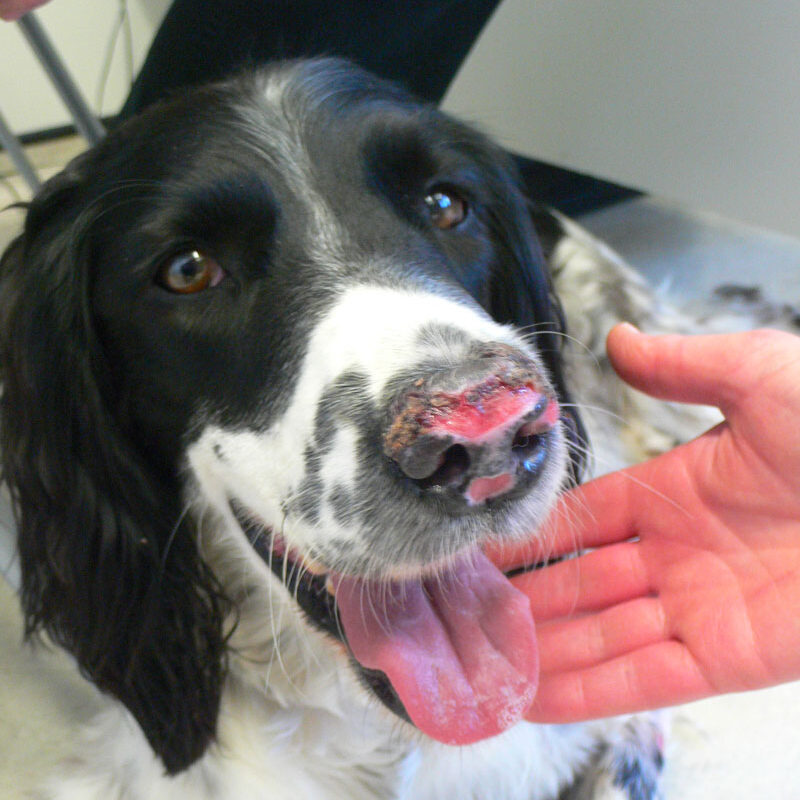
Fig 1: Ulcerative lesions on the nose of a dog with cutaneous vasculitis
What Treatments are Available for Vasculitis?
An important part of the management for cutaneous vasculitis is to identify the underlying cause and correct it. However, once the abnormal immune response has been stimulated, removal of the initial trigger may not be enough on its own.
Drugs to reduce the abnormal immune response are therefore needed in the vast majority of cases, especially in those (idiopathic) cases where no trigger is found. The types of drugs needed depend on the severity of skin lesions present and whether there are any signs of internal organ involvement. In milder cases of vasculitis, mild anti-inflammatory drugs can often be used to control the disease. Where ulcers and bleeding lesions are present, more powerful immunosuppressive medications are usually needed.
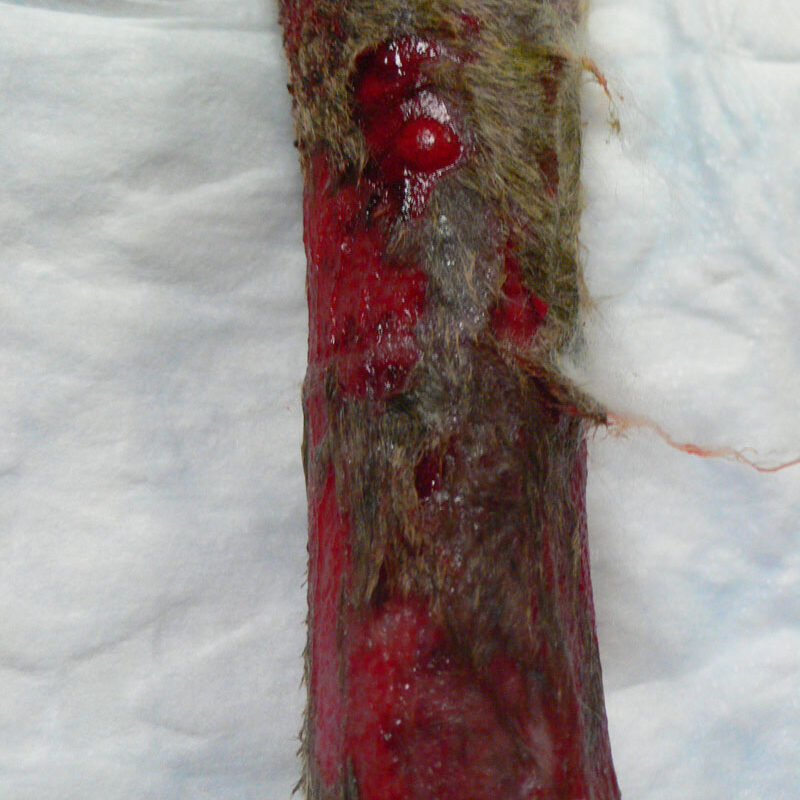
Fig 2: Severe ulcers on the leg of a Greyhound with cutaneous vasculitis
How is Vasculitis Diagnosed?
The disease can be suspected based on the history and clinical signs. Vasculitis usually develops at sites such as the ear tips, nose, lips, tail, inside the mouth and at sites on the paws like the footpads and claws. Lesions also often occur over boney prominences such as the elbows and hocks. When vasculitis is severe and when it occurs suddenly, inflammation results in bleeding and interruption to the blood supply to the skin. Affected animals present with bruising (bleeding into the skin), blisters and ulcers (Figs 1 and 2), and animals are frequently depressed and in pain. In milder cases, where disruption to the blood supply occurs more slowly, clinical signs include hair loss, scaling and scarring.
There are also a number of unique presentations of vascular disease in dogs and cats. An ulcerative form of vasculitis, first reported in Saint Bernard dogs, has been described that remains limited to the septum of the nose. In Greyhounds, a particularly severe form of vasculitis has been reported resulting in ulcerative skin lesions starting on the limbs, and often occurring in conjunction with life threatening kidney disease. Additionally, vasculitis is responsible for a rare syndrome seen in young German Shepherd puppies resulting in swollen, painful and depigmented footpads.
In order to reach a definitive diagnosis, skin biopsies are usually required. Careful selection of biopsy sites is vital to maximise the chances of obtaining the diagnosis. This is because the characteristic signs of vasculitis can be very subtle and temporary, and pathologists have difficulty in reaching the diagnosis if these signs are not seen.
To save this page as a PDF, click the button and make sure “Save as PDF” is selected.
Skin and Ear Clinic
Find out more
To assist owners whose pets have skin and ear conditions, we have put together a range of information pages to talk you through some of the more common dermatology conditions seen by our Specialist team.

