What is Electrochemotherapy?
Electrochemotherapy (ECT) uses short electrical pulses to create temporary holes in the cell membrane that allow drugs to enter into the cancer cell (electroporation). This process results in greater drug uptake by the cell compared to injection or tablets. After the electrical pulses stop, the pores seal allowing the cells to continue to live (reversible electroporation) which is important for normal tissues around the tumour. However, the tumour cells will die due to the effect of the drug that has entered the cell. In larger or more aggressive tumours, repeated higher energy pulses that lead to direct cell death may be used (irreversible electroporation). Tumour cells are more sensitive to electroporation than cells from normal tissues, which explains the low rate of complications in the treated area. ECT does not tend to cause general side effects as the drug concentration in normal cells is low.
How is electrochemotherapy performed?
Patients may receive an intravenous injection of a chemotherapy drug (bleomycin) and/or the tumour or wound itself may be injected with a chemotherapy drug (cisplatin) or calcium chloride. Other drug combinations may be used depending on the type, grade and stage of the tumour. Anti-cancer vaccines or other molecules (e.g. cytokines) can also be delivered with special probes.
Immediately, or a few minutes after injection of these drugs, electrical pulses are administered by electrodes using flat plates on the skin surface or needles placed into the tumour or wound bed (Image1). Typically, very short (millisecond or microsecond) pulses are used and each treatment may last from five minutes to 25 minutes depending on the size of the tumour or surgical wound and the area of the body. Contact between the patient and the electrodes is optimised using an electroconductive gel.
Image 1. Treatment of nasal planum squamous cell carcinoma with plate electrodes. Courtesy of Biopulse s.r.l., Italy
Pulses are generated safely for the operator and the patient using an electroporator certified for veterinary use (Onkodisruptor®) (Image 2). ECT requires brief sedation or general anaesthesia depending on the area treated for the duration of the treatment. Local anaesthetic and painkiller by injection and as tablets are used during the treatment and post-operatively although the procedure results in minimal discomfort.
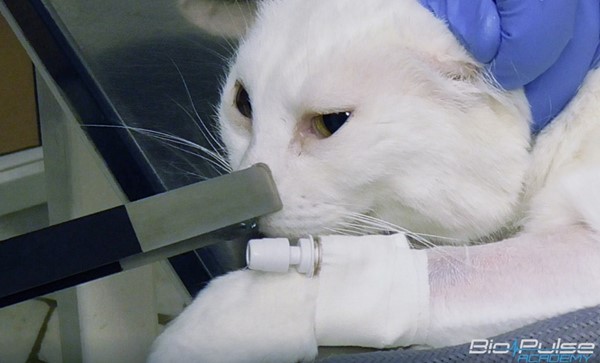

Image 2. Electrochemotherapy device with plate electrodes and needle electrodes. Courtesy of Biopulse s.r.l., Italy
How many electrochemotherapy treatments are needed?
Usually two treatments are given, however occasionally only one or more than two treatments are given, depending on tumour response. Treatments are usually administered two weeks apart although treatment may be delayed depending on tumour response and wound healing. When ECT is used in association with surgery, the first treatment is usually administered within two weeks of surgery. Patients with larger or more aggressive tumours may receive their first treatment during surgery or immediately after closure of the wound.
What are the side-effects of electrochemotherapy?
Electrochemotherapy has little or no functional impact and treated regions heal without damage to healthy tissue. Side effects of ECT are minimal and include redness, swelling and superficial erosion of the skin. During treatment, the electrical current causes temporary muscular contractions, however these contractions do not result in pain or discomfort after recovery and do not require symptomatic therapy. The electrical pulses do not affect electrical activity in the heart.
Insertion of the needles for irreversible electroporation causes a small amount of tissue damage that heals over two to three weeks. Occasionally small burns occur which tend to disappear within two to three weeks and may leave a pink scar. There may be occasional bleeding at the site of insertion of the needles, however this is usually minimal and of short duration.
Local inflammation after treatment may lead to irritation and self-trauma is prevented by wearing a large collar until the wound is healed. Inflammation can be managed by administration of anti-inflammatory painkillers. Patients do not feel unwell after receiving chemotherapy for ECT because the dose is low.
A blood sample is taken to ensure that the patient has a normal red blood cell and white blood cell count and to ensure that treatment has not caused a reduction in the cell counts, although this is very uncommon. Blood tests to ensure that other vital organs (e.g. liver and kidneys) are also performed. Other tests may be recommended if other chemotherapy drugs are used or if the patient’s condition makes this necessary.
When is electrochemotherapy indicated?
Electrochemotherapy (ECT) is indicated for palliative treatment in advanced stage disease, such as tumours with evidence of spread (metastasis) or tumours that cannot be operated on. ECT can also be used to shrink the size of the tumour prior to surgery. However, ECT should not be considered as an alternative to surgery when surgery is possible with a good outcome. ECT can be performed on tumours when they are first recognised or when the tumour recurs after previous surgery, radiotherapy, chemotherapy, or ECT itself.
What tumours can be treated with electrochemotherapy?
Almost any tumour type can be treated with ECT as long as plate or needle electrodes can be applied to it. The most frequently treated tumours are tumours of the skin (e.g. sarcomas, mast cell tumours, carcinomas, melanoma) and tumours of the head and neck (e.g. mouth, ear and nose). Treatment of tumour spread to lymph nodes may also be considered. ECT can sometimes be used via keyhole surgery for tumours in the abdomen.
What is the effectiveness of electrochemotherapy treatment?
Overall, the rate of complete tumour regression following ECT treatment is high although this varies according to tumour type and size. Response to ECT is usually long-lasting, but recurrence may be seen with some tumours. Even in patients with a partial response, ECT can result in a clinical improvement, especially in terms of reduced pain, reduction in bleeding, and reduced need for medical care.
When can electrochemotherapy not be used?
There is currently no known condition which prevents ECT being used. However, patients with other systemic illnesses are assessed individually for any possible increased risk associated with sedation or anaesthesia, and the administration of chemotherapy drugs, and lower doses or different drugs may be used.
Electrochemotherapy is a reliable and versatile treatment that can be performed in virtually any patient, whatever their health status. ECT is rapid, safe and efficient and is a cost-effective treatment that enhances the quality of life of treated patients.
To save this page as a PDF, click the button and make sure “Save as PDF” is selected.
Cancer Care
Find out more
To assist owners in understanding more about Cancer Care we have put together a range of information sheets to talk you through the some of the more common conditions seen and treated by our Specialists.

